A Brief History of Diabetes Technology
Diabetes as a medical condition has been recognised for over 3000 years, however, the technology for managing and monitoring it is still very new in comparison. At Afon we’re at the cutting edge of developing new Diabetes technology which will revolutionise the lives of those living with Diabetes, but what came before our non-invasive continuous glucose monitoring device?
In this article we will take a brief look at the history of Diabetes technology and how it has helped affected people live longer, healthier lives.
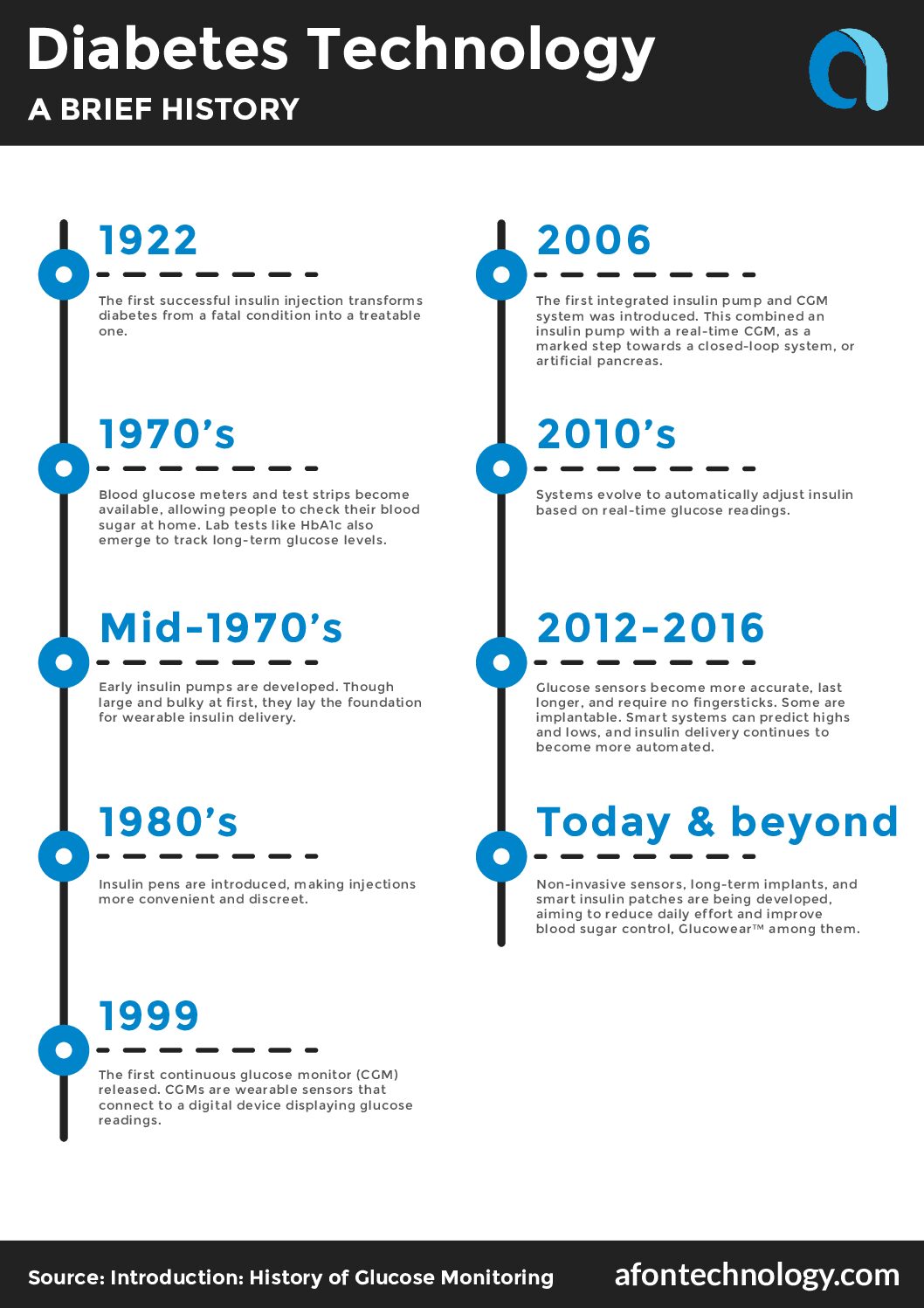
Download a free PDF version of this Timeline of Diabetes Technology.
What is Diabetes?
Diabetes is a very serious condition that causes a person’s blood glucose levels to become too high. This is due to their body not being able to produce enough insulin, any insulin or the insulin isn’t effective.
There are two main types of Diabetes: type 1 and type 2. Type 1 Diabetes is when the body’s immune system attacks and destroys the cell that produce insulin. Type 2 Diabetes is when the body can’t produce enough insulin, or the body doesn’t react very well to insulin.
Glucose is important for everyone’s bodies to function, but it needs to be able to enter our cells to work. When insulin doesn’t work, or isn’t present, the glucose is unable to move from the blood into cells which can lead to painful and life-threatening issues.
Although there is no cure for Diabetes, scientists and doctors have created ways of managing the condition. Giving insulin to Diabetic patients helps get the glucose they need into their cells. Managing Diabetes is a complex, time-consuming, and often frustrating task. However, over the years there have been several different types of Diabetes technology aimed at helping Diabetics. The various types of technology help with the delivery of insulin into their body but also monitoring their blood glucose levels which is critical for self-management.
Diabetes technology before the 1920’s
There are records from ancient Egypt that mention an illness with similar symptoms as type 1 Diabetes; excessive thirst and sweet-smelling urine. We also know that in ancient India, people knew there was an illness associated with glucose by testing urine. Glucose is a form of sugar, so ants would go to urine with a higher concentration of sugar in. Now we know that is because when Diabetic people have too much glucose in their blood, it will also be in their urine.
Over the thousands of years, people worked out there was a difference between Diabetes conditions. They recognised type 1 and type 2 Diabetes were similar but not the same. Unfortunately, there was no technology to help people with Diabetes. No one could figure out it was to do with insulin, or lack of, produced by the pancreas. Indeed, some people thought it was a kidney illness. By the 19th century there was no cure, and no way of managing the illness still. Despite some medicines and diets being prescribed, nothing was very effective, and Diabetes was fatal.
From 1889 there were some major, breakthrough discoveries that changed the lives of people with Diabetes. The discoveries found that Diabetes was in fact connected to the pancreas and it was understood that the pancreas regulated blood sugar levels. This led to some extreme diets being prescribed. Some patients were only allowed to eat 450 calories a day and they often died from starvation before the Diabetes became deadly.
The next breakthrough was the understanding that it was a particular hormone, named insulin, that was the key to glucose leaving the blood and entering cells.
Using insulin as a treatment
Frederick Banting and Charles Best conducted successful trials using insulin on dogs with Diabetes. They isolated insulin and gave it to the dogs which helped them feel better.
The next step was to try this in humans. Frederick and Charles worked with two other scientists called J.B. Collip and John Macleod to purify insulin and test it on human Diabetic patients. The first person to receive an injection of insulin was a 14-year-old boy called Leonard Thompson. According to the American Diabetes Association, “Within 24 hours, Leonard’s dangerously high blood glucose levels dropped to near-normal levels.”
A medical firm called Eli Lilly soon started producing insulin in large quantities, although at this time it was came from cows and pigs. It wasn’t until 1978 that a synthetic insulin was developed and now there are several different types including fast-acting and slow-acting insulin.
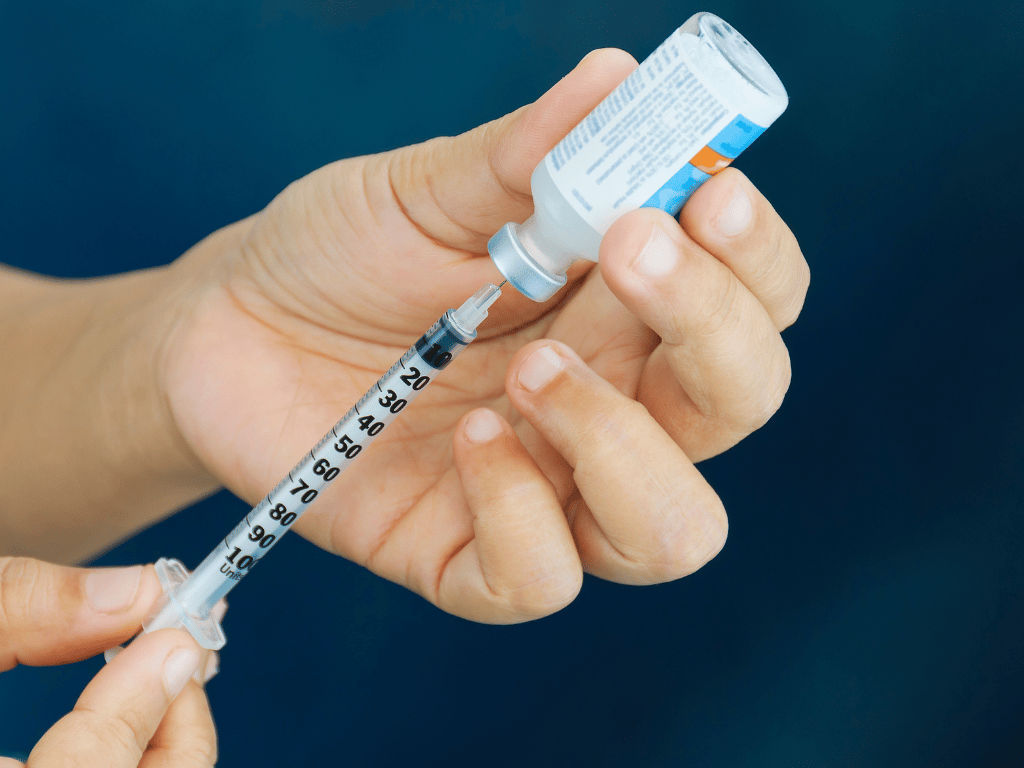
Insulin syringes and pens
At first, insulin was injected into patients with syringes. They were bulky and people needed training on how to use them safely. In the 80’s, the syringes were developed into a more compact device called an insulin pen. These had a dosage setting and replaceable cartridges and were much easier and safer to use.
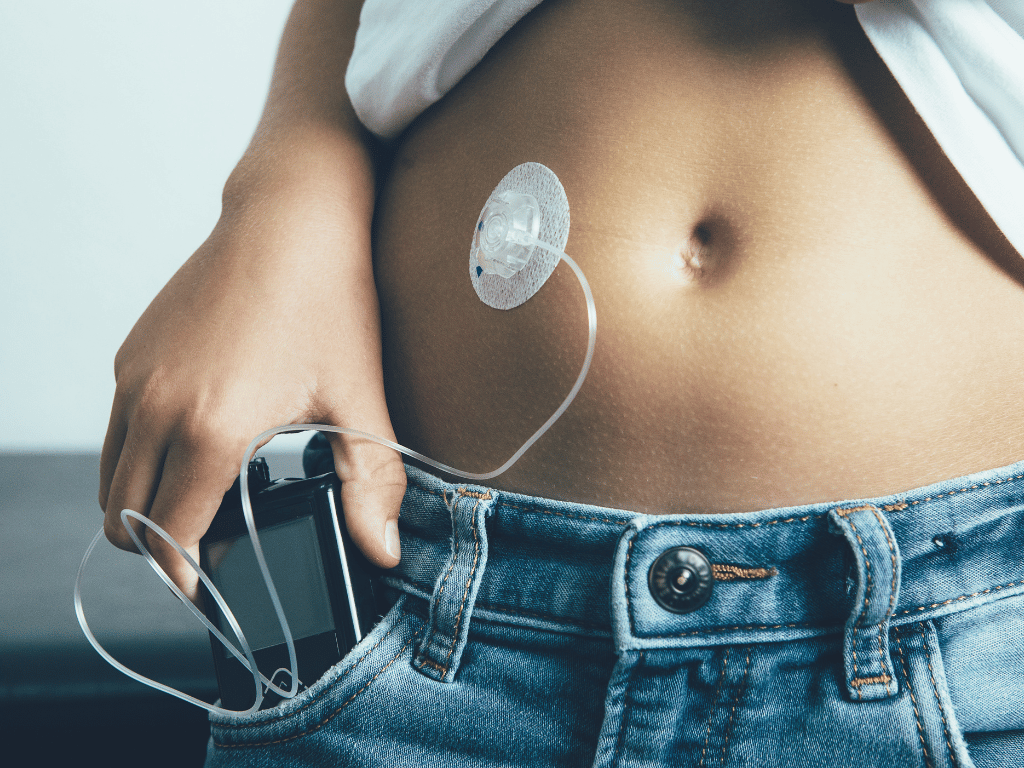
Continuous subcutaneous insulin infusion
The continuous subcutaneous insulin infusion pump, also know as CSII or an insulin pump, was introduced in the 1970’s. It is a battery-operated dispenser with a cartridge of insulin, connected to a catheter. The catheter is inserted into the subcutaneous tissue, the innermost layer of the skin. It delivers insulin without needles, changing the dosage as it measures what is needed continuously.
How the methods of measuring glucose levels changed
Measuring blood glucose levels is a vital part of Diabetes management. Being aware of blood glucose levels enables Diabetics to make informed decisions regarding insulin dosage and food and activity choices.
In 1908, before insulin was discovered, a liquid formula of copper needed to be heated with the patient’s urine to check the glucose levels. This had to be done at the doctor’s surgery or hospital which made it inconvenient. It also meant levels couldn’t be checked as often as we can now. Testing urine remained the best way to check until 1965!
In 1965 a method of testing using blood was invented. A drop of blood would be placed on a test strip and the colour would change, indicating the levels of glucose in the blood. However, this was still only available to doctors meaning patients still couldn’t test their blood glucose at home.
By the 1970’s a home monitor was being investigated, and in the 1980’s the Dextrometer was launched. This had a digital display and used the testing strip previously only available to doctors. Now patients could test at home and throughout the 80’s, the availability of strips grew.
The next two decades saw self-monitoring of blood glucose (SMBG) technology improve until it was recommended for all patients.
Continuous glucose monitors
The first continuous glucose monitor (CGM) was introduced in 1999. However the patient could not view the data, it was only available to their Diabetes clinician. This method of monitoring was very popular though. Although they all needed calibration with a finger prick, new devices that came along were able to notify users of potentially dangerous blood glucose levels in real time.
The next discovery was that blood glucose levels can be measured through a needle into the skin. This meant that CGM’s could be stuck to the skin for a few days at a time. This way of measuring doesn’t need the needle to reach blood. Instead, it measures glucose from the fluid between cells just under your skin, known as interstitial fluid.
More real-time sensors became available from 2004 onwards and in 2012 information could be viewed on a mobile phone.

Diabetes technology 2016 onwards
A new CGM was released in 2016 that did not require constant finger pricking and could be worn for several days with much better accuracy than previous models. Although patients still had to finger prick to calibrate and have CGM’s attached to their skin, it was very much an improvement from 100 years before!
The CGM’s now available show how far Diabetes technology has come in such a short space of time! However, these devices are still invasive, albeit minimally, so the next step for Diabetes technology is a truly non-invasive glucose monitor.
Afon’s Diabetes technology
Afon Technology are developing the future of continuous blood glucose monitoring. Glucowear is non-invasive, meaning there is no finger pricking or sensor needles under the skin. Patients will be able to see their data on their phone, in real-time, making Diabetes management easier than ever before.
The journey of Diabetes technology has been a relatively short but life-changing one. In less than 100 years, Diabetes has gone from being a certain fatal illness to one that can be managed with sufferers able to lead near to normal active healthy lives when their condition is well managed. The technology and discoveries from people all over the world have helped children and adults live longer lives.
Diabetes is a complex illness and all the new technology available is only for managing the condition. There is still no cure. Despite that, Afon Technology will continue their work to provide a convenient, affordable, and non-invasive device to help those living with the condition.

A Brief History of Diabetes Technology FAQs
What is the difference between type 1 and type 2 diabetes?
Type 1 diabetes is an autoimmune condition where the body attacks insulin-producing cells. This is different to type 2 diabetes, which occurs when not enough insulin can be produced by the body, or when the cells don’t respond correctly to the insulin the body does produce (insulin resistance).
How was diabetes recognised and treated before modern technology?
Even as far back as ancient Egypt, diabetes was recognised because the symptoms we associate with diabetes now, were present in people with diabetes then too. Excessive thirst, losing weight without trying, sores that don’t heal, and sweet-smelling urine were all recognisable as an untreatable disease. Sadly, there was no treatment that worked until the medical technology breakthroughs of the 19th century.
What role did the discovery and use of insulin play in transforming diabetes treatment?
Diabetes treatments were truly transformed when the hormone insulin was discovered to impact how glucose interacted with cells. Diabetes went from a fatal to a manageable disease and insulin injections meant that the starvation diets and bogus “cures” were no longer prescribed.
How have glucose monitoring techniques evolved?
Blood glucose monitoring techniques have evolved most rapidly in the most recent two centuries. No longer needing to use ants or dangerous liquid copper, from 1965 we stopped using urine and started testing blood to monitor glucose levels. Advances in digital technology gave diabetes patients the flexibility to test their blood at home with real-time results. When the discovery that interstitial fluid could be used to monitor glucose levels without needing to draw blood, continuous glucose monitors that attached to the skin grew in popularity. Now, CGMs connect to smartphones and continue to deliver real-time results, with regular finger pricking and blood calibration to ensure accuracy.
What makes Afon Technology’s non-invasive Glucowear™ device a game changer in diabetes management?
Using low radio frequency to send a signal into the blood, Glucowear™ is non-invasive which means no needle in the skin all day and night measuring the glucose levels in interstitial fluid. Wearing a CGM device is uncomfortable and comes with hygiene risks and skin irritation. Users can have difficulty finding locations on their body to wear them and CGMs can be knocked or catch on clothing, causing pain. They also need to be replaced regularly adding to the environmental impact of disposable medical waste.
Instead, Glucowear users will simply wear a watch-like device on their wrist and the real-time results will be sent to their smartphone app. No needles, no pain, no rotation of locations, and lasting up to two years without needing replacement.

